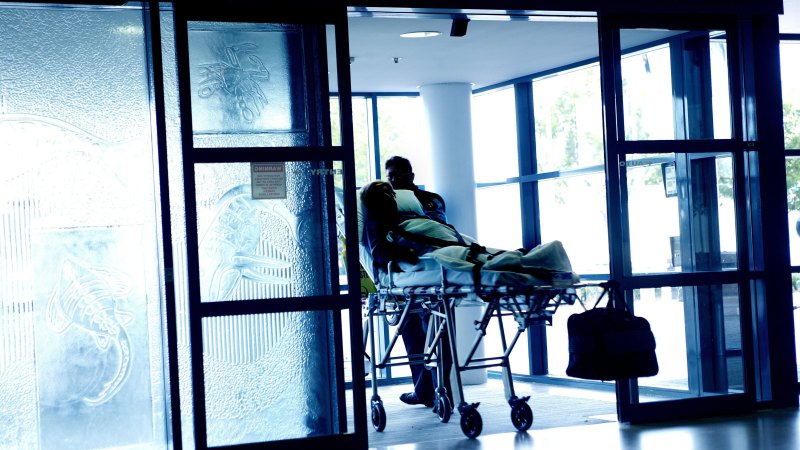
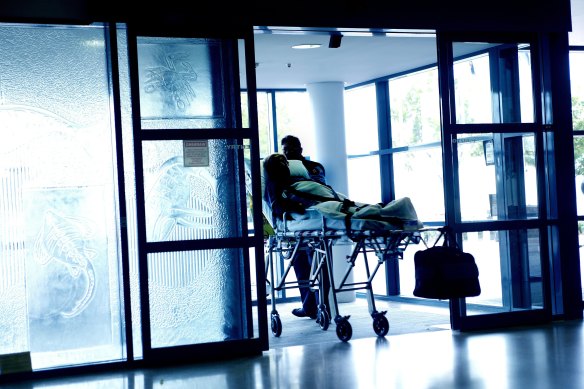
Hundreds of patients died of COVID after catching the virus while being treated at Victorian hospitals for unrelated ailments.
More than 3200 people are suspected to have caught the virus while in hospital between January 1 and October 26 last year, according to leaked Victorian Health Department data. Of these patients, at least 344 – more than 10 per cent – died. Patients in hospitals are particularly vulnerable to COVID infections.
“Infections should not be occurring in healthcare facilities,” said Associate Professor Philip Russo, an infection prevention expert from Monash University.
The data was initially leaked online by an emergency doctor. The Age has independently verified that the information came from an official health department document.
Many hospitals across Victoria have begun winding back pandemic restrictions in recent weeks, including disbanding COVID wards and dropping mask mandates for staff and visitors.
While The Alfred said it was still running a dedicated COVID ward, Austin Health has disbanded its COVID ward and is isolating positive patients in single rooms or with other infected people. The changes are designed to make more beds available as fewer COVID patients present at hospitals.
Hundreds of VIctorians have died after catching COVID while in hospital for unrelated medical issues.Credit:Louise Kennerley
Russo, who sits on a number of infection control groups that advise governments, said removing masks in healthcare facilities was not justified given the high rates of transmission in the community.
“It’s where our vulnerable populations are and we need to continue to protect them,” he said.
Healthscope, which runs dozens of private hospitals including Holmesglen Private Hospital in Moorabbin and the John Fawkner Private Hospital in Coburg, confirmed it had recently dropped its mask mandate for staff and visitors “unless deemed necessary due to clinical indication”.
“These settings are effectively a return to pre-COVID settings, where PPE [personal protective equipment] is used to protect either vulnerable patients, or staff and doctors, against a potential hazard from an infectious patient, with COVID-19 added into existing infection control policies,” a Healthscope spokesman said.
But Australian Nurses and Midwifery Federation Victorian secretary Lisa Fitzpatrick said the easing of mandates was premature.
“The virus is still there and community transmission is increasing,” she said.
The number of people in Victoria hospitalised with COVID surged last week by almost 60 per cent to 183 patients.
A healthcare worker at Box Hill Hospital, which is run by Eastern Health, said COVID positive patients were no longer being segregated from other patients in designated wards. He said they were now placed in private rooms on the general ward.
Professor Peter Collignon says hospitals need to be built with more single beds to prevent cross infections.Credit:Alex Ellinghausen
The recent change was in response to the challenges of opening and closing the COVID-19 ward based on fluctuating case numbers.
“We are miffed by it,” said the worker, who did not want to be identified in case it jeopardised his employment.
“Previously if you were on the COVID ward you knew you were on the COVID ward and you would wear PPE all the time. Now there’s a little bit of COVID floating through the ward.”
A Monash Health spokesman confirmed its health services no longer had COVID wards, and that it cared for patients with the virus using single rooms with negative pressure or flow, which prevents contaminated air from seeping out.
“These rooms have separate ventilation to protect patients, employees, and visitors,” he said.
“Should the number of COVID-positive patient presentations significantly increase, Monash Health will follow its plan to establish a COVID ward.”
Australian Medical Association Victorian president Roderick McRae said he was alarmed so many people had died from COVID after contracting it in hospital.
“It’s a concerning number but plausible,” he said, pointing out that hospital patients were a particularly vulnerable cohort.
Dr Roderick McRae, president of the Victorian branch of the Australian Medical Association.Credit:Joe Armao
The data indicated that those who died of COVID acquired in a hospital tended to be older than patients who caught it in the community, but were less likely to be an aged care resident.
McRae said hospitals were closing COVID wards to free up beds for others who might need them.
“If there are three positive patients in a COVID ward, the other beds can’t be used,” he said.
Victorian Allied Health Professionals Association executive officer Andrew Hewat said surgical masks were still required for clinical areas in public hospitals. Until recently, he said, most health services had required clinical staff to wear N95 respirators, which offer a higher protection than surgical masks.
‘If there are three positive patients in a COVID ward, the other beds can’t be used.’
Hewat said most hospital staff were now only required to wear N95 masks in spaces with very ill patients such as intensive care and emergency wards.
He called on the government to invest more in improving ventilation.
“Personal protective equipment should be the last line of defence, but it has become the primary and often the only defence in most health settings,” he said.
Emergency rural doctor David Berger, who tweeted the leaked data showing definite and probable deaths of patients who had caught COVID in hospital, said it was “scandalous” that hospitals were winding back their precautions against COVID.
“It really crucifies me that we work in an environment where patients are not being safeguarded,” he said.
“This is a widespread illness that has turned the world upside down and remains the third leading cause of death in Australia for 2022. If you catch it in hospital, you’ve got a 10 per cent chance of death.”
Australian National University Professor Peter Collignon, who also sits on numerous infection control committees, said cross infections would continue while patients shared wards.
He said hospitals needed to be built with more single rooms.
“If you’re in a room, sharing a room with somebody who’s got COVID that nobody knows about, you’re basically a metre apart from them, how do you expect him not to get cross infected? And it’s not only for COVID. It’s for influenza and every other respiratory virus as well.”
The Victorian Health Department refused to comment on the data or provide updated figures, and said the information was not publicly available.
Eastern Health was contacted for comment.
The Morning Edition newsletter is our guide to the day’s most important and interesting stories, analysis and insights. Sign up here.
Most Viewed in National
From our partners
Source: Read Full Article